This article was originally published by Pierre-Guy Veer at The Foundation for Economic Education.
*EDITOR’S NOTE: The seizure of and the banning of ownership of private property is one of the tenants of the Great Reset. “You will own nothing and you will be happy.” This is just the beginning. The ruling class will own everything, including you.
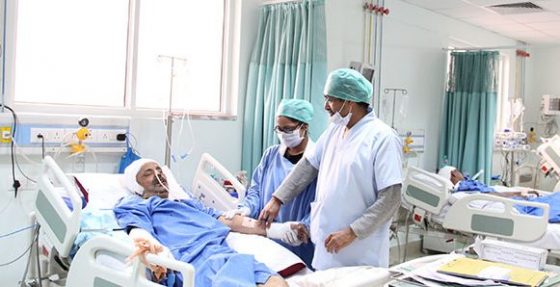
In the Canadian province of Quebec, no party sitting in the provincial parliament dares to question the mammoth size of government. But strangely enough, only one party openly embraces socialism: Québec solidaire (QS). Their motto could be boiled down to “There is no salvation without the State.”
This conclusion is quite obvious when reading a recent Facebook post written by a leader of the left-wing party.
Gabriel Nadeau-Dubois, a co-spokesman for the party who was elected to the provincial legislative assembly in 2017, expressed outrage that it was possible to get an appointment for a “Brazilian butt lift within a few days” while “intensive care units are overwhelmed” because of the COVID-19 pandemic.
Nadeau-Dubois’ team called a few private clinics, and they told him that “there’s no reason to cancel or delay surgeries unless the government tells us otherwise.”
Perhaps inspired by that last point, he proposed seizing private ORs because “an exceptional situation requires exceptional measures… Lives are on the line.”
The Reality of Healthcare Rationing
For a moment, let’s forget the fact that “nothing is more permanent than a temporary government measure,” and that QS is only dreaming about having an all-mighty public sector in nearly every aspect of everyone’s lives.
One has to wonder whether Nadeau has even skimmed through Quebec’s administration of the healthcare system since it was nationalized some 50 years ago. Since the deep cuts of the mid-1990s under Lucien Bouchard, the nominal budget for healthcare has multiplied by a factor of 3.7, increasing five percent per year.
And yet, waiting lists hardly budge.
As of July 2018, the waiting time to see a family doctor was 371 days. These specialists are so overwhelmed that they have already denied service to 75,000 people and counting. As for elective surgeries, over 100,000 people have been on a waiting list for more than six months. Many more patients will have to wait too since “non-urgent” procedures have been delayed because of the pandemic.
What’s more, the province-wide ER occupancy rate is currently 95 percent of available gurneys, with some being well overcapacity. So nothing much has changed over four years ago.
The Major Flaw of Medicare-for-All
Seizing private ORs, or even taxing corporations that “profited from” the pandemic, is very unlikely to shorten waiting lines, however.
As Montreal’s Economic Institute reminds us, Medicare-for-all (Canada has its own version of Medicare) sees people as spending, and therefore they need to be rationed in order not to go over budget.
But in a private hospital, patients are seen as a source of revenue; there is, therefore, an incentive to give great care so that, for future needs, the patient will come back.
And when there is waiting time in private hospitals, it’s rather short compared to their public peers. So much so that public organizations like CSST (Quebec’s OSHA) send workplace injuries to private establishments in order to save time. Indeed, a shorter waiting time means quicker rehab, less spending on worker compensation, etc.
A Strong Motivation to Offer Exceptional Service
So as long as the government funds and administers healthcare, refunding patients using private hospitals could mean saving on precious public funds.
It’s already happening for certain long-term care facilities (CHSLD) that receive public funding but are privately administered. In other words, they work like charter schools, and just like them, they have a sword of Damocles hanging over their heads.
In short: They need to work exceptionally well in order to remain open. Otherwise, the state can easily revoke its license. It’s a strong motivator—especially since public establishments hardly, if at all, suffer the same fate—but it pushes charter school administrators like Alex Quigley in North Carolina to find ways to improve their performance. Through trials and tribulations, Quigley was able to improve his school’s grade from F to D; and he hopes to make it to a C soon.
“Charter” CHSLDs operate in a similar fashion. Since they are publicly financed, they can’t charge users more than the fixed price, which was around $2,000 for a room with one bed in 2020. They even pay income and sales taxes, unlike their 100 percent public counterparts.
And yet, their quality is much better: None of them were evaluated as offering a “preoccupied” level of service compared to 12 percent of their wholly public peers. As for a “very satisfying” level of service, it was respectively 64 percent compared to 18 percent, according to a survey of users.
The improved level of care also probably explains why the only CHSLDs that weren’t contaminated by COVID when it started last year were either charter or entirely private. One head administrator, Marie-Hélène Girard, even went to buy PPE in mid-March 2020 on her own initiative despite severe shortages.
“It wasn’t recommended, but we did it anyway. Better to have those handy than nothing at all,” she said in an interview.
Girard was able to act promptly thanks to a lighter administrative burden. According to economist Pierre Fortin, administrative cost for “charter” CHSLD is 26 percent lower than their 100 percent public counterparts. The overall cost is about 12 percent lower.
A Better Way
So rather than envying the private sector’s efficiency, QS should look at it and take notes. While having no direct out-of-pocket spending can be nice, a median waiting time of 16.3 weeks for medically necessary procedures can lead to a heavy human toll.
Rationing is the result of regulating supply and ignoring prices, profits, and good incentives. “Non-essential” procedures like Lasik or butt lifts either saw price decreases or much slower price increases than regular medical because practitioners saw an opportunity for profit. This drew more providers into the marketplace, which increased supply, driving prices down.
Canadian lawmakers would be wise to emulate the private sector, not co-opt it. By utilizing markets, the private sector has shown it can lower both wait times and costs—something Canada’s “Medicare-for-all” system has failed to deliver.









You want to really mess things up – let a Federal Government run it.
@cranerigger, that’s unfair.We all know our lovely
government always does a great job of running things -into the ground that is!!?
Reality check time.
You cannot “Fight Covid 19”
One can only fall at its feet
and gaze in awe at its pure,
magnificent,indestructible.
and complete godliness?
Q.Does the prez Bidet administration have an opinion on the Canadian proposal of seizing private hospitals to fight the phantom menace?
A.I’m um gonna um have um
to um circle um back um on um that.? “Jen”
Something which you pay-for and operate, under external controls, is slavery and tribute — not a partnership.
a brief overview in communist takeover of privately owned vital services.
especially, important for those needing critical wound care during the Great Reset.
Pol Pot
The Cambodian genocide (Khmer: ហាយនភាពខ្មែរ or ការប្រល័យពូជសាសន៍ខ្មែរ) was the systematic persecution and killing of Cambodians by the Khmer Rouge under the leadership of Communist Party general secretary Pol Pot, who radically pushed Cambodia towards communism. It resulted in the deaths of 1.5 to 2 million people from 1975 to 1979, nearly a quarter of Cambodia’s 1975 population (c. 7.8 million).[1][2][3]
Joseph Stalin
Stalin instituted the Great Purge, (Reset)
in which over a million were imprisoned and at least 700,000 executed between 1934 and 1939. By 1937, he had complete personal control over the party and state.
Stalin’s government promoted Marxism–Leninism abroad through the Communist International and supported European anti-fascist movements during the 1930s,
Chairman Mao
His policies resulted in the deaths of tens of millions of people in China during his 27-year reign, more than any other 20th-century leader; estimates of the number of people who died under his regime range from 40 million to as many as 80 million,[262][263] done through starvation, persecution, prison labour and mass executions.[188][